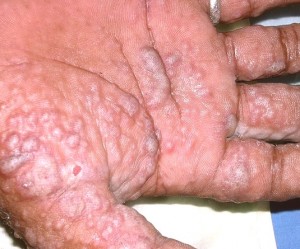
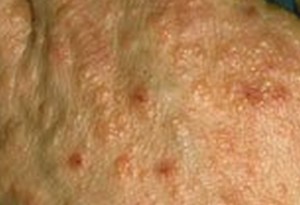
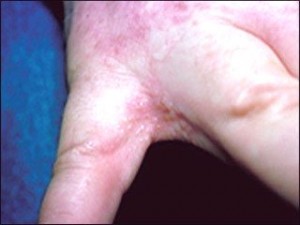
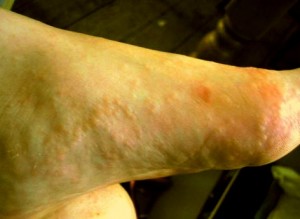
What is dyshidrotic eczema? This is also known as dyshidrosis or pompholyx and is a condition of the skin where small blisters that are fluid filled (vesicles) occur on the palms of the hands or the soles of the foot or both
These blisters that occur usually last somewhere around 3 weeks and creates itching that is very intense. Once these blisters dry, grooves and cracks (fissures) form, that can be very painful.
Symptoms of Dyshidrotic eczema
With this condition, the skin affected becomes inflamed – dermatitis. Therefore, the junctions between the cells of skin open and let fluid – serum – fill the spaces. Physicians refer to this procedure as “spongiosis” since when viewed under a microscope; the skin turns out to be more sponge-like with these fluid-filled spaces.
Symptoms and signs of dyshidrotic eczema include:
• Itchy small bumps which are gradually progressing into a rash made up of blisters that are fluid-filled – vesicles
• Itching that is intense
• Groove or cracks – fissures – on the toes or fingers
• Pain – particularly with blisters that are large
• The small blisters – filled with fluid are commonly found on the fingers as well as the palm of the hand
• Also can occur on the soles as well as the toes of the feet
• Blisters last 3 weeks
If an individual has a rash on the hands or feet that does not leave on its own, call your primary care physician. Also contact your physician if you have been diagnosed with this condition and the symptoms or signs of an infection develop including:
• Fever
• Pain
• Inflammation at the rash site
Causes
The cause of dyshidrotic eczema is not known. But, it may be linked with a comparable skin condition known as atopic dermatitis as well as allergic situations, such as hay fever or asthma – allergic rhinitis. In individuals with allergies, outbreaks may be seasonal.
Risk factors for Dyshidrotic eczema
• Being women. Females seems to have this eczema in higher incidence
• Stress. This disorder seems to be most common during stressful times
• Contact to metal salts. These consist of cobalt, nickel as well as chromium – normally thru mechanical or cement work
• Have periodic allergies. One instance is hay fever
• Contact with moisture. Skin is frequently exposed to water or other wet ingredients – can activate this eczema.
For the majority of individuals, dyshidrotic eczema is merely an inconvenience that is itchy. But for some, the itching and pain can limit the use of their hands. In other cases, skin damage – including thickening of the skin – or an infection by bacteria might occur due to the sponge-like, open skin or the concentrated scratching. This may make treatment more difficult and last longer.
Diagnosis and tests of Dyshidrotic Eczema
In the majority of cases, the primary care physician can make a diagnosis based merely on a physical exam.
Potassium hydroxide (KOH) test
The doctor might advise a procedure called a KOH test in order to exclude any other conditions, for instance contact dermatitis or fungal infection. This test is performed by the physician scraping the skin with a glass slide and collecting dead skin cells. These skin cells are then mixed with KOH or potassium hydroxide and looked at under a microscope to help rule out fungal infection.
Allergy patch test.
When an allergy is believed to cause this disorder, a patch test might help to determine the probable cause. With a patch test, allergens that are suspected are applied to a patch which is placed on the skin in order to check for any reaction.
Treatment for dyshidrotic eczema
Any plan of treatment for dyshidrotic eczema might include:
• Ointments or creams with corticosteroid. The physician may advise corticosteroid topical creams that are high-potency in order to hurry the disappearance as well as improve the blister appearance and to manage the fissures and cracks occurring once the blisters are dried. With cases that are severe, the physician might prescribe steroids to take orally.
• Compresses. Cold or wet compresses might help to improve itching, and increase the efficiency of the topical creams as well as minimize the blisters.
• Antihistamines. The physician may also advise anti-itching drugs called anti-pruritics or anti-histamines, like diphenhydramine or Benadryl and loratadine or Clariten, Alavert, to aid with the itching.
• Phototherapy. If treatments are not effective, the physician might advise a special ultraviolet light treatment called “psoralen plus ultraviolet A” or PUVA. With this treatment exposure to ultraviolet light combined with drugs aid in making the skin more amenable to the effects of the ultraviolet light. There is a newer kind of ultraviolet B light identified as “narrow-band ultraviolet B” that also can help.
• Ointments that are immune suppressing. These drugs, such as tacrolimus or Protopic and pimecrolimus or Elidel, might be useful if other options have not worked. But due to the fact that this subdues the immune system, infections of the skin may be very likely.
• Botulinum toxin injections. Some physicians might consider using botulinum toxin injections especially to treat severe cases. But, this is a comparatively new treatment option that has not gained wide spread acceptance with all physicians.
Yes. I am not sure if they have an app.
My webpage; Skipthedishes Voucher